Pavilion Publishing and Media Ltd
Blue Sky Offices Shoreham, 25 Cecil Pashley Way, Shoreham-by-Sea, West Sussex, BN43 5FF, UNITED KINGDOM
Lyme disease: diagnosis and treatment in general practice
bs_subtitle
It is important for GPs to be aware of the increasing problem of Lyme disease in the UK, which is no longer confined to remote rural areas.
Lyme disease, or Lyme borreliosis, is the most common vector-borne disease in the northern hemisphere with a steadily increasing incidence.
It is an infectious disease caused by the bacterium Borrelia burgdorferi, a spirochaete passed to humans by the bite of an infected tick. Lyme disease is classed as a zoonosis because infection can pass from animals to humans via ticks. Ticks become infected after feeding on the blood of animals, especially small rodents such as mice, which act as the main reservoir for Borrelia in nature. Larger animals such as deer have natural immunity, but facilitate tick mating and the spread of ticks over large geographical areas.
In the UK there are approximately 1,000 laboratory-confirmed cases per year, which is probably an underestimate of the true incidence.1
Most laboratory-confirmed cases are from the English southern counties and Scotland, but cases occur throughout the country, including towns and cities.
Lyme disease affects males and females equally, and in the UK those in the 45-65 year age-group appear to be more at risk. Anyone whose work or lifestyle brings them into regular contact with ticks, including foresters, game-keepers, walkers, cyclists and gardeners, may be at increased risk. Each year around 10-15% of cases are thought to be contracted abroad, from the USA or mainland Europe. Currently, Lyme disease is not notifiable, but occupationally acquired infections are reportable under RIDDOR (Reporting of Injuries, Diseases and Dangerous Occurrences Regulations 2013, Health and Safety Executive).
In Europe, there are at least five genospecies of Borrelia burgdorferi that cause human infection:2
- Borrelia garinii: associated with neurological disease
- Borrelia afzelii: associated with skin infection and an atypical neurological presentation3
- Borrelia burgdorferi sensu stricto: associated with arthritis and the main cause of Lyme disease in the USA, also occurs in Europe
- Borrelia spielmanii
- Borrelia bavariensis.
It is important for GPs to be aware of the increasing problem of Lyme disease in the UK, which is no longer confined to remote rural areas. Tick awareness with prompt effective tick removal is vital in preventing Lyme disease. Increasing public concern about ticks and Lyme disease means that patients may consult their GP at any stage from tick-bite to late-stage disease. Early diagnosis and treatment with antibiotics have a better outcome, whereas diagnosis and treatment of late-stage Lyme disease can be challenging.
Following a tick bite, what are the risks?
It only takes one bite from a tick infected with Borrelia to transmit Lyme disease. Only around one in three people notice a tick bite and most UK ticks do not carry Borrelia. A recent study analysing B. burgdorferi in nymph ticks across the southern counties of England found between 0 and 14% infected.6 The relative risk of contracting the disease from a single tick bite is thought to be low, particularly where there is awareness of risk, and the ticks are removed within 24 hours.7
What are ticks?
Ticks are arachnids and resemble small spiders. After mating, female ticks lay around 2,000 eggs, which progress through three stages: larva, nymph then adult, each stage taking a single blood meal before moulting to the next life stage. They are found throughout the UK in woodland, moorland and urban parks and gardens with sufficient humidity, and wildlife on which to feed. Ticks are most active during the spring, summer and early autumn from March to October when people are likely to be involved in outdoor activities. In addition to B. burgdorferi, ticks may sometimes carry a range of other pathogens that cause disease in humans. Travellers to Europe, especially Eastern Europe, should be warned about the risk of tick-borne encephalitis virus (TBEV), for which there is an effective vaccine.
Ticks bites are relatively painless and not itchy as the ticks inject anti-inflammatory and anti-clotting agents while continuing to feed over several days (usually up to 5 days). The nymph stage, which is when ticks most commonly bites humans, is very small and may go unnoticed. In adults tick-bites usually occur on the lower body, such as the lower leg or groin. In small children bites are mainly seen on the upper body, particularly the head, neck and around the hairline.4
The risk of Lyme disease transmission increases the longer an infected tick remains attached.5 Tick checks with prompt and effective tick removal using tweezers or tick removal tool are important for prevention.
How should ticks be removed?
Ticks should be removed by using a tick removal tool and following manufacturers’ instructions, or fine-tipped tweezers. If using tweezers, grasp the tick firmly, as close to the skin as possible, and pull straight out.
The Lyme Disease Association sell tick removal tools in their shop (http://www.lymediseaseaction.org.uk/what-we-are-doing/shop/), while they are also available in some vets and pharmacies. It is recommended to pack a tick removal tool in a family first aid kit, while they are also small enough that they can easily be carried in a wallet or handbag. Plastic tick removal tools such as the O’Tom hook and Tick-card are lightweight and easy to take abroad.
Please note:
- You should not use fingernails, smother with petroleum jelly or attempt to burn the tick
- The area should be cleaned afterwards with an antiseptic
- Further information should be provided regarding early symptoms of Lyme disease and advise return in case of further symptoms.
Are prophylactic antibiotics recommended?
Since the risk of contracting Lyme disease from a single tick-bite in the UK is thought to be low, prophylactic treatment with antibiotics is not recommended. However, a GP may wish to consider and take advice on prophylactic treatment if a patient is immunocompromised or has visited a more highly endemic area, such as the north-eastern USA or Eastern Europe. Prophylaxis with single dose antibiotics is currently not recommended in the UK.
What are the early signs of Lyme disease?
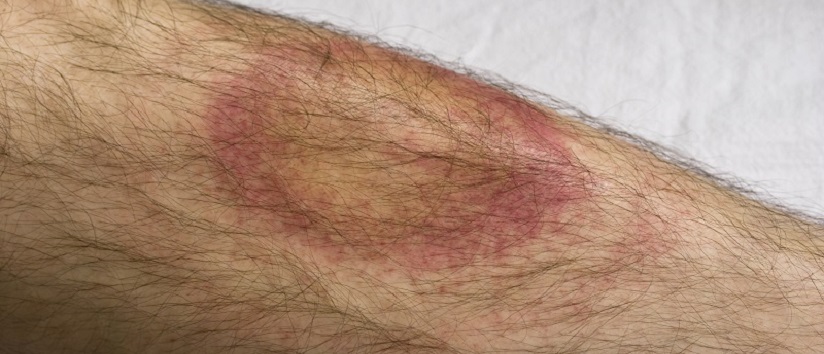
An important early diagnostic sign is the erythema migrans rash (EM), a gradually expanding rash with central clearing which may resemble a ‘bull’s eye’. In the UK only around 65% of people notice this.8 The disease may be diagnosed clinically at this stage and treated successfully with antibiotics by the GP without the need for blood tests.
Additionally, erythema migrans:
- Generally, occur 3-30 days after the tick-bite
- Is usually not particularly itchy or painful like insect and mosquito bites
- Is not scaly like ringworm (tinea)
- The rash may be atypical in appearance, homogenously red or ‘bruise-like’ in appearance
- Rashes may be multiple and distant from the bite-site, suggesting early dissemination.
Flu-like symptoms such as headache, fatigue, migratory arthralgia/myalgia, nausea, low-grade fever and malaise may occur due to immune activation. If the EM rash is absent, awareness of this presentation as an atypical ‘summer-flu’ may be a vital clue to early diagnosis.
Additional signs may include mild fluctuating cognitive problems, sound/light sensitivity, anxiety and panic attacks.
Lyme disease generally does not present with respiratory symptoms and in many cases, fever and lymphadenopathy may be absent.
What is the clinical picture in late Lyme disease?
Lyme disease can spread over the course of weeks and months to the nervous system, joints, heart, eyes and other organs causing a chronic, debilitating multi-system disorder.
Relapsing-remitting malaise, fatigue and headache may accompany a wide range of other symptoms. In Europe, where there is greater diversity of Borrelia genospecies, late-stage Lyme disease is associated with neurological problems, whereas the American form of the disease mainly causes arthritis, especially mono-articular arthritis of large joints such as the knee, and more severe systemic disease.9 Lyme carditis tends to present at an early stage with varying degrees of heart block. Less commonly, eye involvement leads to conjunctivitis, uveitis and a range of other ophthalmic problems. A chronic skin lesion called acrodermatitis chronicum atrophicans (ACA) occurs mainly in Eastern Europe.10
What is Lyme neuroborreliosis (LNB)?
In the UK around 15-25%, people may go on to develop Lyme neuroborreliosis.8 This can affect the peripheral, central and autonomic nervous system.
The typical neurological picture in adults is known as “Bannwarth’s syndrome:11
- A slowly progressive radiculitis causing sensory symptoms with neuropathic pain, paraesthesia and sensory loss. Motor symptoms may include weakness or paralysis
- Cranial neuritis most commonly of the facial nerve (VII) causing facial palsy, but may involve other cranial nerves
- Aseptic meningitis, with minimal neck stiffness.
Autonomic problems include postural orthostatic tachycardia (POTS) with dizziness, headache and orthostatic intolerance.12 Subtle neuro-cognitive problems can lead to slowness of information processing, word finding difficulty and memory problems.13
Children may develop aseptic meningitis and facial palsy, possibly bilateral. Headache, fever and facial palsy occurring in children during the peak Lyme disease season between May to October may indicate Lyme disease.14 In younger children, non-specific symptoms such as irritability, loss of appetite and weight loss may be the only sign.15
How is Lyme disease diagnosed?
Diagnosis should be clinically supported where necessary by test results. It is important to enquire about the risk of tick exposure, tick-bite or rash with a careful record of evolving signs and symptoms.
Symptoms may be non-specific and overlap with a range of other conditions, including multiple sclerosis, Bell’s palsy, Guillain-Barre syndrome, Parkinson’s disease, stroke, dementia, and autoimmune conditions such as SLE, rheumatoid arthritis and sarcoidosis as well as psychiatric conditions: anxiety, panic attacks, mood disorders, psychosis and obsessive-compulsive symptoms. The relapsing remitting pain and fatigue may resemble chronic fatigue syndrome, ME or fibromyalgia.
What tests are used for Lyme disease?
Lyme serology, which aims to detect the antibody response to Borrelia, may be negative in the first few weeks because antibodies take time to develop. In the UK, a first tier ELISA or EIA is followed by a second tier immunoblot if the ELISA is positive or equivocal, or there is a strong clinical suspicion of Lyme disease. It is important to be aware that Lyme serology tests have inherent limitations.16,17 There is currently no test for disease activity or cure.
A positive result can indicate past infection and a negative result may not necessarily exclude a diagnosis. Lumbar puncture may be carried out to further investigate suspected Lyme neuroborreliosis. The clinical use of PCR to directly detect the DNA of Borrelia is limited to use in skin, synovial tissue biopsies or CSF because of limited sensitivity.18
Routine blood tests and inflammatory markers are usually normal.
Given the limitations of current Lyme disease diagnostics, definitive serological diagnosis of Lyme disease may not be possible on an individual patient basis. If a GP remains concerned that the history and symptoms indicate a probable or possible diagnosis of Lyme disease, even despite standard early treatment, there is the option to contact the National Lyme Reference Laboratory at PHE Porton for discussion of detailed test results and advice (01980 612348) and also Lyme Disease Action ([email protected]).
How is Lyme disease treated?
All stages of Lyme disease respond to treatment with antibiotics, though early treatment with oral antibiotics is associated with a better outcome. Erythema migrans should be treated with antibiotics immediately without waiting for the results of serology tests, which are likely to be negative at this early stage.
NICE guidance states:
| Symptoms | Treatment | First alternative | Second alternative |
| Lyme disease without focal symptoms | |||
| Erythema migrans and/or
Non-focal symptoms |
Oral doxycycline:
100 mg twice per day or 200 mg once per day for 21 days |
Oral amoxicillin:
1 g 3 times per day for 21 days |
Oral azithromycinb:
500 mg daily for 17 days |
| Lyme disease with focal symptoms | |||
| Lyme disease affecting the cranial nerves or peripheral nervous system | Oral doxycycline:
100 mg twice per day or 200 mg once per day for 21 days |
Oral amoxicillin:
1 g 3 times per day for 21 days |
N/A |
| Lyme disease affecting the central nervous system | Intravenous ceftriaxone:
2 g twice per day or 4 g once per day for 21 days (when an oral switch is being considered, use doxycycline) |
Oral doxycycline:
200 mg twice per day or 400 mg once per day for 21 days |
N/A |
| Lyme disease arthritis | Oral doxycycline:
100 mg twice per day or 200 mg once per day for 28 days |
Oral amoxicillin:
1 g 3 times per day for 28 days |
Intravenous ceftriaxone:
2 g once per day for 28 days |
| Acrodermatitis chronica atrophicans | |||
| Lyme carditisb | Oral doxycycline:
100 mg twice per day or 200 mg once per day for 21 days |
Intravenous ceftriaxone:
2 g once per day for 21 days |
N/A |
| Lyme carditis and haemodynamically unstableb | Intravenous ceftriaxone:
2 g once per day for 21 days (when an oral switch is being considered, use doxycycline) |
||
Some patients develop a Jarisch-Herxheimer reaction (JHR) after starting antibiotic treatment with a transient worsening of symptoms. This occurs as a result of the inflammatory response when bacteria are targeted and killed, with a worsening of fever, chills, muscle pains and headache.
Currently, the optimum treatment for disseminated or late Lyme disease is unknown and further research is needed.11 Relapse and treatment failure requiring re-treatment have been documented,19 as has persistence of bacterial infection after antibiotic treatment.20,21
What is the prognosis for late Lyme disease?
Over 50% of people who go on to develop Lyme neuroborreliosis experience significant residual symptoms.22 This can result in significant disability and seriously affect quality of life.23
The cause of persistent symptoms following treatment is poorly understood and may involve immune dysfunction,24 bacterial persistence21,25 and tissue damage, including damage to neural networks.26
What needs to happen to improve services for Lyme disease patients?
A number of improvements have been identified:
- Further research is required to establish the true scale of the problems related to Lyme disease and other tick-borne diseases in the UK
- Increased public awareness of the health risk from ticks and Lyme disease in the UK to improve prevention
- Research on better tests and treatments for those diagnosed at a later stage, and new tests aimed at very early diagnosis
- Commissioning of specialist services with special expertise in diagnosis and treatment
- Improved medical awareness and education.
Suggested resources
- Lyme Disease Action is a national registered charity working to raise awareness of Lyme disease and associated tick-borne diseases, and the need for better tests, prevention and treatment. http://www.lymediseaseaction.org.uk/
- Public Health England: https://www.gov.uk/government/collections/lyme-disease-guidance-data-and-analysis
- Public Health England suggested referral pathway for patients with symptoms related to Lyme disease: http://webarchive.nationalarchives.gov.uk/20140714084352/http:/www.hpa.org.uk/webc/HPAwebFile/HPAweb_C/1317141297288
- NICE Clinical Knowledge Summaries for Lyme disease: http://cks.nice.org.uk/lyme-disease
- Lyme disease: NICE guidance: https://www.nice.org.uk/guidance/ng95
- RCGP elearning module on Lyme disease: http://elearning.rcgp.org.uk/course/info.php?id=164
Dr Sandra Pearson, Lyme Disease Action
References
- Medlock JM, Leach SA. Lancet Infect Dis 2015; 15: 721-730.
- Stanek G, Wormser GP, Gray J, et al. Lancet 2011; 6736: 13.
- Strle F, Ruzic&-Sabljic& E, Cimperman J, et al. Clin Infect Dis 2006; 43: 704-10.
- Robertson JN, Gray JS, Stewart P. Eur J Epidemiol 2000; 16: 647-652.
- Cook MJ. Int J Gen Med 2015; 1-8.
- Hansford KM, Fonville M, Jahfari S, et al. Epidemiol Infect 2014; 1-9.
- Tijsse-Klasen E, Jacobs JJ, Swart A, et al. Parasit Vectors 2011; 4: 17.
- Lovett JK, Evans PH, O’Connell S, et al. Epidemiol Infect 2008; 136: 1707-11.
- Cerar T, Strle F, Stupica D, et al. Emerg Infect Dis 2016; 22: 818-27.
- Stanek G, Fingerle V, Hunfeld K-P, et al. Clin Microbiol Infect 2011; 17: 69-79.
- Mygland A, Ljøstad U, Fingerle V, et al. Eur J Neurol 2010; 17: 8-16, e1-4.
- Kanjwal K, Karabin B, Kanjwal Y, et al. Cardiol J 2011; 18: 63-6.
- Fallon BA, Nields JA. Am J Psychiatry 1994; 151: 1571-83.
- Nigrovic LE, Thompson AD, Fine AM, et al. Pediatrics 2008; 122: e1080-5.
- Broekhuijsen-van Henten DM, Braun KPJ, Wolfs TFW. Arch Dis Child 2010; 95: 910-4.
- Ang CW, Notermans DW, Hommes M, et al. Eur J Clin Microbiol Infect Dis 2011.
- Lee ang MMG, Ang CW, Berkhout J, et al. The diagnostic accuracy of serological tests for Lyme borreliosis: a systematic review and meta-analysis. 2016.
- Wilske B, Fingerle V, Schulte-Spechtel U. FEMS Immunol Med Microbiol 2007; 49: 13-21.
- Dillon R, O’Connell S, Wright S. Clin Med 2010; 10: 454-7.
- Preac-Mursic V, Wilske B, Gross B, et al. Infection 1989; 17: 355-359.
- Rudenko N, Golovchenko M, Vancova M, et al. Clin Microbiol Infect 2015; 22: 267.e9-267.e15.
- Eikeland R, Mygland A, Herlofson K, et al. Acta Neurol Scand 2011; 1-6.
- van den Wijngaard CC, Hofhuis A, Harms MG, et al. Eur J Public Health 2015.
- Chandra A, Wormser G, Klempner M, et al. Brain Behav Immun 2011; 24: 1018-1024.
- Sharma B, Brown A V, Matluck NE, et al. Antimicrob Agents Chemother 2015.
- Ramesh G, Benge S, Pahar B, et al. J Neuroinflammation 2012; 9: 72.