Pavilion Publishing and Media Ltd
Blue Sky Offices Shoreham, 25 Cecil Pashley Way, Shoreham-by-Sea, West Sussex, BN43 5FF, UNITED KINGDOM
In recent years, obesity has become a global epidemic that places an enormous burden on healthcare resources. Obese individuals, more specifically those with abdominal obesity, often exhibit risk factors that lead to cardiovascular or metabolic diseases. Such cardiometabolic risk factors are of great concern in the elderly given the changes that occur with ageing (notably sarcopenia), decreased metabolic rate and decreased physical activity, all of which contribute to increased weight gain.
Double trend: obesity and ageing
In the UK, the proportion of men and women categorised as obese (body mass index [BMI] over 30 kg/m2) increased from 13.2 per cent in 1993 to 23.6 per cent in 2004, and from 16.4 per cent in 1993 to 23.8 per cent in 2004, respectively1. A quarter of the adult population is projected to become obese by 20102. Parallel to this increase in obesity, the longevity of individuals and the average age of the overall population are increasing – the geriatric population is now one of the fastest growing segments of the population in Europe and the US. In the UK, it is estimated that a fifth of the population is over 60 years of age, and by 2025 the number of people over the age of 80 years is set to increase by almost 50 per cent, with the number of people over the age of 90 years doubling3. These two increasing trends – ageing population and obesity – therefore, have major public health implications. Furthermore, it must be noted that up to the age of 74 years, there is a positive association between age and weight gain; after this age a slight decline is observed4.
Changes in body composition
Ageing is associated with considerable changes in body composition; notably, fat mass increases while lean mass decreases5. However, it is not just the increase in fat mass that is of concern, but importantly, it is the location where the excess fat is deposited. With ageing, the accumulation of abdominal, or visceral fat, is quantitatively and proportionally greater than peripheral fat mass5. The reason why visceral fat is specifically affected is not clearly understood; however, it has been suggested that hormonal changes may be a contributing factor. In women, a decline in oestrogens with menopause has been identified as an independent factor associated with the accumulation of visceral fat. Correspondingly, a decline in testosterone in men is associated with abdominal obesity5 .
The other major change in body composition with ageing is sarcopenia. Sarcopenia refers to the loss of skeletal muscle mass and strength that starts as early as the fourth decade of life in humans6. It is one of the major causes of morbidity in the elderly and contributes signifi cantly to the decrease in their quality of life6. In addition to contributing to the functional limitations of old age, sarcopenia has a number of signifi cant metabolic consequences. Notably, there is an increase in the lipid content of skeletal muscle, both inside and outside the skeletal muscle fi bres7. This increase in lipid deposition has been linked to the development of insulin resistance7. Furthermore, as muscle mass takes up approximately 30 per cent of resting energy expenditure, reduction in muscle mass and decreased physical activity in the elderly leads to a decrease in total energy expenditure6. This decline leads to other co-morbidities, including obesity and visceral fat accumulation6.
Abdominal obesity: a significant risk factor
Cardiometabolic risk factors are those that lead to cardiovascular and metabolic diseases, and include abdominal obesity, dyslipidaemia, hypertension, glucose intolerance and insulin resistance. Of these cardiometabolic risk factors, abdominal obesity – or more specifically excessive visceral fat – plays a significant aetiological role in the development of cardiovascular and metabolic disease, and contributes to the development and exacerbation of other cardiometabolic risk factors8; consequently, it is critical to differentiate between obesity and abdominal obesity. BMI is a commonly used measure of obesity; however, it has inherent limitations, as it does not differentiate between lean and fat tissue.
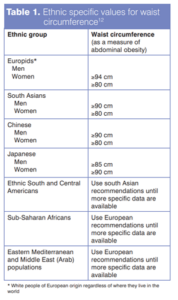
Waist circumference (WC) is a measure of abdominal fat, and consequently a better screening measure for cardiometabolic risk than other anthropometric indicators9-11. Indeed, a new defi nition of metabolic syndrome proposed by the International Diabetes Federation (IDF) includes central obesity as an essential criterion, given the strong evidence linking WC with cardiovascular and metabolic diseases12. Furthermore, the IDF provides different WC cutoffs for people from different ethnic gro ups (see Table 1)12. WC should be measured with a tape measure from halfway between the lowest point of the ribs and the diac crest. As acknowledged by the IDF, a growing body of evidence indicates individuals with abdominal obesity are at increased risk of type 2 diabetes11, cardiovascular disease – including coronary heart disease13, hypertension14 and myocardial infarction15 – and overall mortality16. Ideally, therefore, WC must be used in conjunction with BMI in primary care.
Cardiometabolic risk
Results of the Health Survey of England 2003 revealed that increased waist/hip ratio (WHR) and WC showed a more pronounced relation with age than obesity, both peaking at a later age than obesity4. Therefore, the groups identified as being at risk by having increased WHR or WC contain a substantially greater proportion of older people than the group defined as obese4.
In a large prospective study, elderly individuals (age range 70–79 years) with high risk WC were almost twice as likely as those with a low risk WC to develop chronic heart failure17. This increased risk was independent of obesity, inflammation, hypertension and diabetes, indicating that excess visceral fat per se is likely to be responsible for the heart failure17. Given that age increases cardiometabolic risk, the presence of abdominal obesity and sarcopenia exacerbate the problem significantly. Furthermore, achieving the targets set for cardiometabolic risk factors according to current guidelines can be extremely difficult in the elderly and, in most instances, polytherapy is necessary. For example, cardiometabolic risk factors with difficult-to-achieve targets include hypertension, dyslipidaemia and elevated HbA1c. Consequently, targeting visceral fat, which can cause or exacerbate these risk factors, can be viewed as pivotal to reducing the cardiometabolic risk profile of elderly patients.
Cardiometabolic risk management
Primary care physicians can potentially play a significant role in implementing an integrated screening and intervention approach to address key risk factors in the general population. According to guidelines recently published by the Joint British Societies, all patients above the age of 40 years should be considered for an opportunistic comprehensive cardiovascular disease risk assessment18. Those with a 10-year cardiovascular risk of greater than 20 per cent should be targeted for aggressive risk factor management18.
Lifestyle intervention is an integral aspect of managing and reducing cardiometabolic risk in any age group. Moderate weight loss and increased physical activity can improve physical function and quality of life in obese elderly individuals. Therefore, prescribing a diet with calorie reduction and lower consumption of saturated fat could be valuable. However, it is important to note that if a diet is prescribed, it should be ensured that adequate protein intake is included to counteract reduced muscle mass as low protein intake is not uncommon, particularly in the elderly. In addition, recommended light exercise should focus on building lean body mass with resistance training.
Implementation of cardiometabolic risk reduction will necessitate an increase in the prescribing of agents such as statins and anti-hypertensives to address the relevant, individual risk factors. In the elderly, who may already be receiving polytherapy, further increasing the number of tablets they need to take can be challenging for them. Consequently, a single agent that targets the overall cardiometabolic risk, rather than the individual components, can be of enormous benefit.
Pharmacological intervention to decrease abdominal obesity is indeed an option to be considered for the management of cardiometabolic risk. A number of agents are currently available for the treatment of obesity, notably orlistat and sibutramine. Orlistat prevents the absorption of fat molecules from the gastrointestinal tract, while sibutramine promotes a feeling of satiety19,20. According to guidance from the National Institute for Clinical Excellence (NICE), these drugs should be used in individuals with a BMI of ≥30 kg/m2, or those with a BMI ≥28 kg/m2 (≥27 kg/m2 for sibutramine) and other risk factors that persist despite standard treatment (for example, type 2 diabetes, high blood pressure and/or high total cholesterol level)19, 20. However, both have limitations in that sibutramine cannot be prescribed to patients over the age of 65 years and orlistat to those over 75 years19,20. Therefore, there is a need for long-term management of cardiometabolic risk in the elderly.
Rimonabant is a novel agent recently licensed in the UK for the management of cardiometabolic risk factors. It is indicated as an adjunct to diet and exercise for the treatment of obese patients (BMI ≥30 kg/m2), or overweight patients with a BMI >27 kg/m2 with associated risk factors such as type 2 diabetes and dyslipidaemia. In clinical trials, rimonabant has been shown not only to reduce weight and WC, but also improve other cardiometabolic risk factors. Notably, it significantly improves glycaemic control in people with diabetes, and improves lipid profile by significantly increasing high density lipoprotein cholesterol and decreasing triglyceride levels in people with treated or untreated dyslipidaemia21,24. The improvements in cardiometabolic risk factors are, to a certain extent, independent of the effect of rimonabant on weight loss.
Conclusion
Obesity is an increasingly important problem in the elderly and should not be merely considered as ‘middle-age spread’. The changes in body composition that occur have significant clinical implications – visceral fat accumulates and muscle mass (protein) decreases, while concomitantly, the lipid content of skeletal muscle increases. These metabolic changes, in conjunction with decreased physical activity, lead to a significantly increased cardiometabolic risk profile in the elderly.
Overall, there is a need for greater physician involvement in the management of cardiometabolic risk factors that frequently manifest in abdominally obese patients in primary care. Achieving the targets set for cardiometabolic risk factors according to current guidelines can necessitate polytherapy in many elderly individuals. Therefore, in this population, the use of a single agent, such as rimonabant, that targets the common underlying pathophysiological cause rather than using multiple therapies to treat individual cardiometabolic risk factors can be of benefit.
Key points:
- The prevalence of obesity is rising rapidly in the UK.
- Obesity, particularly abdominal obesity, is associated with increased cardiometabolic risk.
- Measurement of waist circumference is a relatively quick and easy measure of increased abdominal obesity, and hence a marker of increased cardiometabolic risk.
- Lifestyle change remains the key intervention to reduce obesity.
- Pharmaceutical interventions may be necessary in addition to lifestyle changes for some patients.
Dr Azhar Farooqi GP, East Leicester Medical Practice
Conflict of interest: Dr Farooqi has been a member of the professional advisory boards of several pharmaceutical companies in relation to therapies for diabetes.
References
- Health Survey for England 2004 – latest trends. Available at http://www.ic.nhs.uk/pubs/ hlthsvyeng2004upd/ 2004trendcommentary.pdf/fi le. Accessed March 2006
- National Audit Office. Tackling Obesity in England. 2001. Available at http://www.nao.org.uk/publications/nao_reports/00- 01/0001220.pdf. Accessed March 2006
- Department of Health. National Standard Framework for older people, 2001. Available at http://www.dh.gov.uk/assetRoot/ 04/07/12/83/04071283.pdf Accessed July 2006
- Health Survey for England 2003. Available at http://www.dh.gov. uk/assetRoot/04/09/89/09/0409 8909.pdf. Accessed March 2006
- Beaufrere B, Morio B. Fat and protein redistribution with aging: metabolic considerations. Eur J Clin Nutr 2000; 54 (Suppl 3): S48–53
- Karakelides H, Sreekumaran Nair K. Sarcopenia of aging and its metabolic impact. Curr Top Dev Biol 2005;68: 123–148
- Janssen I, Ross R. Linking agerelated changes in skeletal muscle mass and composition with metabolism and disease. J Nutr Health Aging 2005; 9: 408–419
- Després JP, Lemieux I, Prud’homme D.Treatment of obesity: need to focus on high risk abdominally obese patients. BMJ 2001; 322: 716–720
- Wei M, Gaskill SP, Haffner SM, Stern MP. Waist circumference as the best predictor of noninsulin dependent diabetes mellitus (NIDDM) compared to body mass index, waist/hip ratio and other anthropometric measurements in Mexican Americans – a 7-year prospective study. Obes Res 1997; 5: 16–23
- Janssen I, Katzmarzyk PT, Ross, R. Body mass index, waist circumference and health risk. Arch Intern Med 2002; 162: 2074–2079
- Wang Y, Rimm EB, Stampfer MJ, et al. Comparison of abdominal adiposity and overall obesity in predicting risk of type 2 diabetes among men. Am J Clin Nutr 2005; 81: 555–563
- Alberti KG, Zimmet P, Shaw J. The metabolic syndrome – A new worldwide defi nition. Lancet 2005; 366: 1059–1060
- Rexrode KM, Carey VJ, Hennekens CH, et al. Abdominal adiposity and coronary heart disease in women. JAMA 1998; 280: 1843–1848
- Harris MM, Stevens J, Thomas N, et al. Associations of fat distribution and obesity with hypertension in a bi-ethnic population: the ARIC study. Atherosclerosis Risk in Communities Study. Obes Res 2000; 8: 516–524
- Yusuf S, Hawken S, Ounpuu S, et al. INTERHEART Study Investigators. Effect of potentially modifi able risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 2004;364: 937–952
- Kuk J, Katzmarzyk PT, Nichaman MZ, et al. Visceral fat is an independent predictor of allcuase mortality in men. Obesity 2006; 14: 336–341
- Nicklas B, Cesari M, Penninx B, et al. Abdominal obesity is an independent risk factor for chronic heart failure in older people. J Am Geriatr Soc 2006; 54: 413–420
- JBS 2: Joint British Societies’ guidelines on prevention of cardiovascular disease in clinical practice. Heart 2005; 91; 1–52
- Orlistat for the treatment of obesity in adults. Guidance No 22, National Institute for Clinical Excellence, 2001
- The clinical effectiveness and cost effectiveness of sibutramine for obesity. Guidance No 22, National Institute for Clinical Excellence, 2001
- Pi-Sunyer FX, Aronne LJ, Heshmati HM, et al; RIO-North America Study Group. Effect of rimonabant, a cannabinoid-1 receptor blocker, on weight and cardiometabolic risk factors in overweight or obese patients: RIO-North America: a randomized controlled trial. JAMA 2006; 295: 761–775
- Despres JP, Golay A, Sjostrom L; Rimonabant in Obesity-Lipids Study Group. Effects of rimonabant on metabolic risk factors in overweight patients with dyslipidemia. N Engl J Med 2005; 353: 2121–2134
- Van Gaal LF, Rissanen AM, Scheen AJ, et al; RIO-Europe Study Group. Effects of the cannabinoid-1 receptor blocker rimonabant on weight reduction and cardiovascular risk factors in overweight patients: 1-year experience from the RIO-Europe study. Lancet 2005;365: 1389–1397
- Scheen A. Rimonabant in Patients with Type 2 Diabetes: Results from the RIO-Diabetes Trial. Abstract 750221, presented at the 65th American Diabetes Association meeting, 2005. Personal communication


